THE DIFFERENCE BETWEEN ORAL AND GENTIAL HERPES
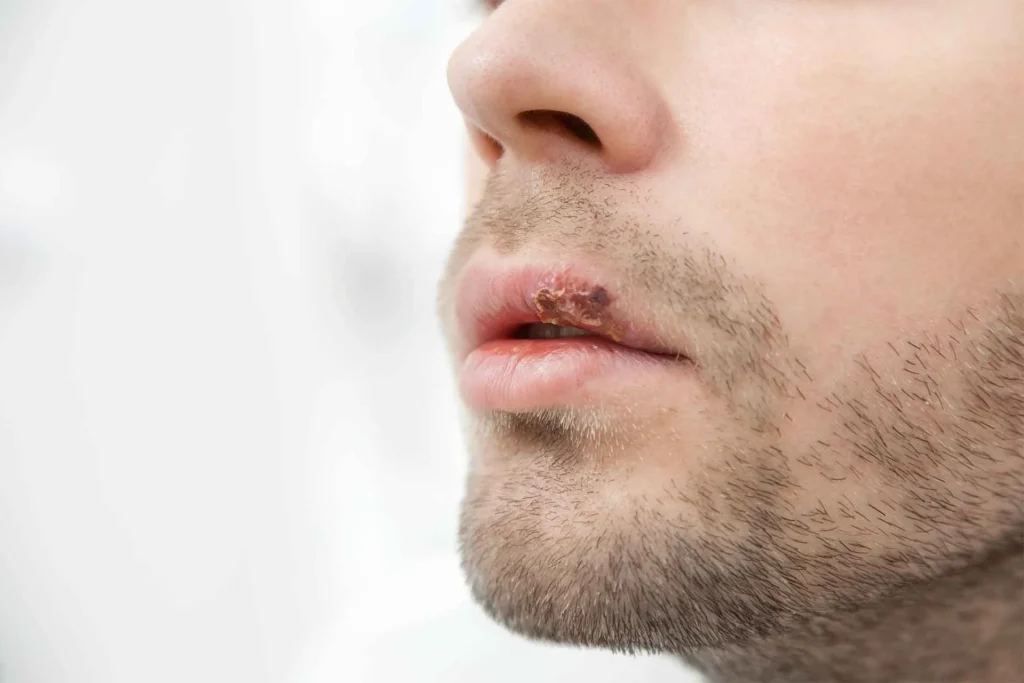
Although there are technically eight different viruses in the herpes family, the most relevant and commonly known are herpes simplex virus 1 (HSV1) and herpes simplex virus 2 (HSV2). HSV1 is responsible for the majority of cold sores, or fever blisters. These sores begin as water blisters that open, crust over and then heal. They typically occur two to three times per year often in conjunction with another illness, such as a cold, hence the term “cold sore”. Cold sores are commonly located on the lips, nose and chin.
Meanwhile, HSV2is the main culprit for recurrent genital herpes. Symptoms of genital herpes include blisters, sores, itchiness, cracks, ulcers or irritation of the skin, pain during urination, watery discharge from the penis or vagina and pain running down the legs. Non-genital symptoms include headache, sensitivity to light, swollen lymph nodes, low grade fevers and nerve pain. HSV2 inhabits a group of nerves at the base of the spine which allows the symptoms to occur anywhere in the boxer short area. Outbreaks can occur on the buttocks, hips, thighs, lower abdomen, anus and genitals. The location of an outbreak can change from outbreak to outbreak or remain constant.
TRANSMITTING HERPES AND VIRAL SHEDDING
HSV1 can also cause genital herpes. In fact, HSV1 accounts for almost 40% of all new genital herpes infections in the U.S. An HSV1 genital infection is the result of mouth-to-genital transmission. HSV1 genital outbreaks recur infrequently – about once every other year or less.
Transmission can occur when the virus is shedding which means that an active outbreak does not need to be present in order to transmit the virus. When HSV1 is located genitally, it sheds one to two days per month which is far less often in comparison to HSV2. When located orally, HSV1 sheds at a much higher rate, nearly 33% of the time. Because of HSV1’s affinity for the mouth, almost half of all HSV1 genital cases will have no recurrent outbreaks at all.
Like HSV1, HSV2 can occur orally or genitally. Over 90% of recurrent genital herpes is from HSV2 because HSV1 has a very low recurrence rate when located genitally.HSV2 is almost always transmitted from genital-to-genital contact. Transmission can occur during shedding which typically occurs up to 12 days out of the month regardless of if a lesion is present or not. When located orally, HSV2 only sheds about 1% of the time because HSV2 has an affinity for the genitals. HSV2 reoccurs genitally about three to five times per year. About 20% of cases have more than 10 recurrences each year. Over time, those affected have fewer recurrences, but the shedding of the virus does not change.
IDENTIFYING HERPES OUTBREAK TRIGGERS
Researchers have not been able to pinpoint all of the HSV1 oral outbreak triggers, but one they are certain of is sunlight. Developing a cold sore a few days after hiking or spending time at the beach is common. Using SPF lip balm may reduce the number of fever blisters that occur. Trauma is also a known outbreak trigger which is why pre-visit forms for medical and dental procedures usually ask if a patient has a history of herpes. Trauma can be as minor as simple dental work or lip fillers, so if a patient checks “yes”, they will likely be advised to use antiviral therapy for a week or so before the procedure so that recovery will not be complicated by a cold sore. Other outbreak triggers include stress, lack of sleep, spicy foods, change in time zones, and prolonged oral sex.
There are no well-documented triggers for genital herpes, butsome theories include stress, illness, lack of sleep, specific foods, menstrual periods and friction from sexual intercourse. Similar to oral herpes, trauma such as lower abdominal or back surgery can also trigger an outbreak because the nerves in which the virus is located are disrupted. Anything that suppresses the immune system, such as steroids may also result in increased vulnerability to outbreaks.
THE STIGMA SURROUNDING HERPES OTHER SEXUALLY TRANSMITTED INFECTIONS
Our society has held on to a stigma in addition to deeply negative views towards sexually transmitted infections (STIs). No one is eager to pass herpes on to someone else. In fact, the biggest fear most people have is giving the virus to someone else. But, the truth is that most people have herpes. Nearly 90% of people who have HSV2 do not know that they are infected. About 56% of people over the age of 14 in the U. S. have HSV1 and about 20% have HSV2. Females are more likely to have HSV2 because transmission is easier and more efficient for the receiving partner during intercourse. Statistically speaking, a greater number of sexual partners increases the likelihood of contracting herpes. If you test positive for either HSV1 or HSV2, you can spread the virus to someone else regardless of whether or not you have symptoms.
HOW OFTEN DOES HERPES SHEDDING OCCUR?
| HSV 1 oral shedding | Up to 33% of days |
| HSV 1 genital shedding | 5% of days |
| HSV 2 genital shedding | Up to 40% of days |
| HSV 2 oral shedding | 1% of days |
HOW TO CURE HERPES
Unfortunately, there is no cure for HSV1 or HSV2. Antiviral medication can be taken orally to decrease shedding rates. To date, the leading treatment is Ozone IV therapy. Treatment should begin once prodrome, or early symptoms start and continue daily until the symptoms are gone. Ozone IV therapy may take three to five cycles until outbreaks are completely eradicated or reduced to an acceptable rate. Most of the time, Ozone IV therapy can stop herpes symptoms entirely though they can reappear years later in times of stress.
True healing begins at the root. If you’re ready for a personalized, root-cause approach to your health, we invite you to contact our office to schedule a consultation.